Ever tried to swing a racket or lift a coffee mug, only to feel a sharp twinge in your elbow that said, âNope, not todayâ? That sensation may be lateral epicondylitis–more commonly referred to as tennis elbow–announcing its presence like an uninvited guest. It's a pesky condition that doesn't just haunt tennis players, as anyone who overuses their forearm muscles can be affected. Whether it's from typing, gardening, tennis, or some other activity, that nagging pain can make daily life a drag. But the good news is that there's hope, and it doesn't require needles or surgery.
Physical therapy is like a trusty sidekick for tackling tennis elbow. With the right techniques, therapists can help ease the pain, get your arm moving smoothly again, and keep you in your game–whatever that might be. One study is worth discussing because it highlights how a hands–on therapy technique often administered by physical therapists outshined cortisone injections in the long run. Let's unpack this study and see how physical therapy can help you wave goodbye to your elbow woes.
Hands–on therapy clearly outperforms injections for tennis elbow
Tennis elbow occurs when the tendons in your forearm–tough bands that connect muscle to bone–get overworked and irritated near the outside of the elbow. Overstraining these tendons is a gradual process that's caused by any activity that involves repetitive motions. While tennis elbow is the most common culprit, swinging a hammer, painting walls, or even scrolling on your phone too long can also be responsible. Statistics show that up to 3% of adults deal with tennis elbow each year, and while it's most common in folks aged 30â50, it can occur at any age.
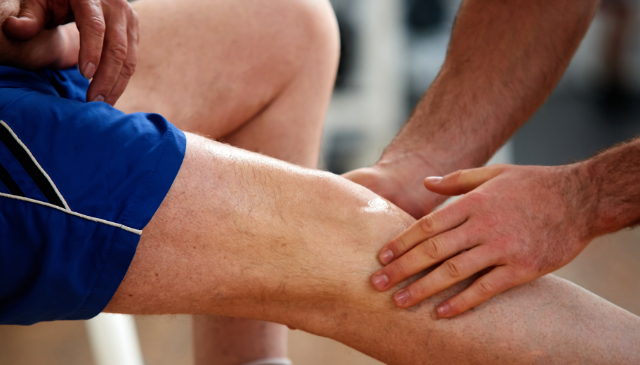
With this in mind, a study was conducted to compare the effectiveness of deep friction massage to steroid injections for treating tennis elbow. Deep friction massage is a hands–on–or manual–therapy technique in which a physical therapist applies deep, targeted pressure with the fingertips across the grain of muscles, tendons, or ligaments to increase blood circulation and maintain or restore mobility. Researchers wanted to get a better idea of what works best for this stubborn condition, since treatments like splints and steroid shots don't always deliver lasting relief. They found 34 patients who had tennis elbow for at least 6 weeks and split them into the following three groups:
- Group 1: these patients wore a wrist splint for six weeks and did stretching exercises after a rest period
- Group 2: these patients received an injection of cortisone (a steroid used to reduce inflammation) and followed the same splint–and–stretch plan as Group 1
- Group 3: these patients received deep friction massage–which involved firm, circular rubbing of the sore spot on the elbow–followed by the same splint–and–stretch routine as Group 1
Researchers then evaluated pain, arm function, and grip strength at 6â12 weeks and 6 months after these interventions.
What did the results show?
All patients experienced relatively similar improvements at 6â12 weeks after the interventions. Pain decreased to a similar extent in all three groups, while Groups 2 and 3 reported better arm function and stronger grip strength than Group 1. But by 6 months, patients in Group 3 who underwent massage therapy had significantly greater improvements than the other two groups. Their pain dropped significantly, while arm function and grip strength both soared. Groups 2 and 3, on the other hand, did not retain the initial improvements, as neither pain, function, nor grip strength were much different at 6 months than 6â12 weeks.
Translating findings into action with personalized physical therapy
These results are important because they spotlight how cortisone injections are not a sustainable long–term solution. These shots often provide immediate pain relief, but this relief fades fast and can even make things worse down the line by weakening tendons. Meanwhile, deep friction massage seems to activate the healing process–likely by boosting blood flow and/or breaking down scar tissue–without those risks.
Physical therapists are big supporters of hands–on interventions like massage. They frequently use manual therapy techniques like joint mobilization (gentle nudges to loosen joints) and manipulation (bolder adjustments) and often toss in massage techniques like deep friction to calm those fussy tendons. Collectively, these techniques facilitate the healing process in the elbow to alleviate pain and improve function.
Call us today for a chance to experience lasting relief
Don't let tennis elbow bench you from the things you enjoy, whether that's tennis, gardening, or something else entirely. This study shows that deep friction massage can be a long–term game–changer, and our physical therapists are ready to use these effective techniques for your elbow.
Give us a call today if you have any questions or you're ready to schedule your first appointment. For those of you interested in learning more about the study, click here.